Heart Health · Cardiology · Treatment Guidelines
Acute Pericarditis Treatment Guidelines: Symptoms, Causes, Diagnosis & Latest 2025 Treatments
- What acute pericarditis is and how common it is worldwide
- What causes heart sac inflammation and who is at risk
- Key symptoms — and how to tell it apart from a heart attack
- How doctors diagnose pericardial inflammation
- The latest 2025 ACC & ESC treatment guidelines — step by step
- Possible complications, prevention tips, and when to go to the ER
1. What Is Acute Pericarditis?
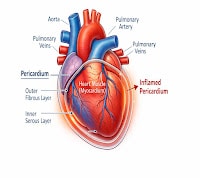
Your heart sits inside a thin, two-layered sac called the pericardium. This sac protects your heart and holds it in place. When this sac gets inflamed — doctors call it heart sac inflammation or pericardial inflammation.
When it starts suddenly and lasts less than 6 weeks, doctors call it acute pericarditis. It is one of the most common causes of sharp chest pain in young adults aged 16 to 40.
The good news? 70–90% of patients recover fully — without serious problems — when treated early and correctly. Do not ignore symptoms. Early care makes all the difference.
Bottom line: Most people who get proper treatment walk out of the clinic feeling fine within 2–3 weeks.
2. What Causes Acute Pericarditis?
Most of the time, a viral infection is the culprit. Think of the last time you had a bad cold or flu — that same virus can sometimes travel and inflame the sac around your heart. In many cases though, no specific cause is ever found. This is known as idiopathic pericarditis — which simply means the cause is unknown.
| Category | Common Examples | Notes |
|---|---|---|
| Viral (Most Common) | Coxsackievirus, Echovirus, COVID-19, Influenza, EBV | Up to 90% of cases in developed countries |
| Bacterial | Tuberculosis (TB), Staphylococcus, Streptococcus | More serious; higher risk of complications |
| Autoimmune | Lupus (SLE), Rheumatoid Arthritis, Sjogren’s Syndrome | Common in young women; treat root condition first |
| Post-cardiac Injury | After heart attack, heart surgery, cardiac procedures | Can appear days to weeks after the event |
| Medications | Hydralazine, Procainamide, Isoniazid | Stops when the medicine is discontinued |
| Other | Kidney failure, Cancer, Radiation therapy | Harder to treat; specialist care needed |
Who Gets It Most?
Young men between 16 and 40 years old are most affected — though this condition does not spare women or older adults. People who recently had a viral illness, COVID-19, heart surgery, or those living with autoimmune diseases like lupus are at higher risk. A previous episode also raises the chance of it happening again.
The takeaway: A simple viral infection is behind most cases. Knowing your risk helps you act faster if symptoms appear.
3. What Are the Different Types of Pericarditis?
Not every case of pericarditis looks the same. The type depends mainly on how long symptoms last and whether they come back:
| Type | Duration | What It Means |
|---|---|---|
| Acute | Less than 6 weeks | First episode; most common and usually self-limiting |
| Incessant | More than 6 weeks, continuous | Symptoms do not fully go away after the first episode |
| Recurrent | Returns after 4–6 weeks of no symptoms | Affects 15–30% of patients if undertreated |
| Chronic | Lasting more than 3 months | Less common; may lead to constrictive pericarditis |
Worth knowing: Most first-time patients have the acute type and recover fully. Recurrence is usually the result of stopping treatment too early.
4. What Are the Symptoms of Acute Pericarditis?
Imagine waking up at 2 AM with a sharp, stabbing pain in your chest — one that gets worse when you lie back down, but eases slightly when you sit up and lean forward. That is the classic presentation of acute pericarditis. Many people rush to the ER thinking it is a heart attack. But the pain pattern is quite different.
Beyond chest pain, patients commonly experience a low-grade fever, unusual tiredness, shortness of breath when lying down, and sometimes a dry cough. Some feel their heart racing or beating irregularly. Pain can also radiate to the left shoulder or neck — which is why this condition gets mistaken for so many other things.
Pericarditis vs Heart Attack — Key Differences
| Feature | Pericarditis | Heart Attack |
|---|---|---|
| Pain type | Sharp, stabbing | Pressure, squeezing, crushing |
| Lying flat | Makes it worse | No change |
| Leaning forward | Makes it better | No change |
| Deep breath | Makes it worse | No change |
| Age group | Young adults (common) | Older adults (more common) |
| Troponin levels | Usually normal or slightly raised | Significantly elevated |
If your chest pain improves when you lean forward — do not wait. See a doctor the same day.
5. How Do Doctors Diagnose Acute Pericarditis?
There is no single test that confirms pericarditis on its own. The diagnosis is pieced together — symptoms, a physical exam, and test results all matter. At least two of the following signs must be present:
- Pleuritic chest pain — sharp, worse with breathing or lying down
- Pericardial friction rub — a scraping sound your doctor hears through a stethoscope
- Electrocardiogram changes — a specific pattern called saddle-shaped ST elevation
- Fluid around the heart (pericardial effusion) seen on imaging
- Raised inflammation markers in blood — especially CRP
- Pericardial swelling visible on Cardiac MRI
Tests Your Doctor Will Run
ECG (Electrocardiogram)
Usually the first test ordered. It shows a distinctive saddle-shaped ST elevation pattern — and helps rule out a heart attack quickly.
Blood Tests
CRP is the most important marker — it confirms active inflammation and tells the doctor when it is safe to stop treatment. Troponin is also checked to see if the heart muscle is affected.
Echocardiogram (Echo)
A heart ultrasound. It checks for fluid buildup around the heart and makes sure the heart is pumping normally.
Cardiac MRI
Ordered when the diagnosis is unclear. It uses a special dye to highlight inflamed areas around the heart — giving doctors a clear picture that other tests cannot. The 2025 guidelines now strongly recommend it for complex cases.
Chest X-Ray
Not specific for pericarditis — but useful to rule out pneumonia, lung problems, or a significantly enlarged heart.
For most patients, an ECG and a simple CRP blood test are enough to confirm the diagnosis and start treatment the same day.
6. Treatment Guidelines (2025) ACC 2025 · ESC 2025
The good news about treatment is that it is straightforward for most patients. The 2025 guidelines from the ACC and ESC agree on one thing: two medicines together work far better than one alone.
First-Line Treatment — For Almost All Patients
Most patients start feeling noticeably better within just a few days of starting this combination. The pain eases, fever drops, and energy slowly returns.
| Medicine | Dose & Duration | Why It Is Used |
|---|---|---|
| Ibuprofen (NSAID) | 600 mg every 8 hours for 1–2 weeks | Reduces pain and swelling. Always take with food. |
| Aspirin | 750–1,000 mg every 8 hours for 1–2 weeks | Preferred if patient already takes aspirin for heart disease. |
| Colchicine | 0.5 mg twice daily (>70 kg) or once daily (<70 kg) for 3 months | Cuts the chance of recurrence by 50%. Never skip doses. |
| Omeprazole (PPI) | 20–40 mg daily alongside NSAIDs | Protects the stomach lining. Always pair with NSAIDs. |
What About Exercise?
This is the part most patients find frustrating — but it is non-negotiable. No intense physical activity for at least 1 month. The inflamed pericardium is sensitive. Pushing through exercise too early can worsen swelling and trigger a relapse.
When First-Line Treatment Does Not Work
A small number of patients do not respond to NSAIDs and colchicine. In those cases, the approach depends on what is driving the inflammation:
| Situation | What Doctors Recommend |
|---|---|
| High CRP + fever — first medicines failed | Anti-IL-1 medicines (Rilonacept or Anakinra) — block the protein driving heart sac swelling. Now preferred over steroids per ACC 2025. |
| Cannot take NSAIDs (kidney disease, stomach ulcer) | Low-dose Prednisone — start at the lowest effective dose, taper slowly |
| Autoimmune-related (Lupus, Rheumatoid Arthritis) | Treat the root condition first. Pericarditis often resolves along with it. |
| Condition keeps returning | Colchicine extended to 6 months. Anti-IL-1 medicines if still not controlled. |
The 2025 Breakthrough — Anti-IL-1 Medicines
Rilonacept and Anakinra are the biggest additions to the 2025 guidelines. They work by blocking a protein called IL-1 — think of it as a fire alarm inside the body that keeps triggering inflammation. These medicines switch that alarm off. Clinical trials showed faster recovery, fewer relapses, and a good safety record. The ACC now recommends them ahead of steroids for patients who need second-line therapy.
Who Actually Needs to Be Admitted?
In many cases, patients leave the same day with a prescription. But hospital admission is needed when things are more serious — large fluid buildup around the heart, severe uncontrolled pain, high fever above 38°C, signs of heart muscle involvement, or if the patient is pregnant, immunocompromised, or on blood thinners.
Ibuprofen + Colchicine + rest. That is the core of treatment for nearly everyone — and when followed correctly, it works very well.
7. What Is the Outlook for Patients?
The outlook is genuinely positive for the large majority of people. With the right treatment, 70–90% recover fully within 1–3 weeks. Those who stop medicine early — usually because they feel better — are the ones most likely to see it come back.
Constrictive pericarditis — where scar tissue forms and squeezes the heart — is very rare in viral cases, affecting less than 1%. It is more of a concern with bacterial or TB-related pericarditis, where early hospital care makes a significant difference in outcomes.
People who follow their treatment plan — and attend follow-up appointments — almost always come out the other side feeling completely normal.
8. What Can Happen If Pericarditis Is Left Untreated?
Ignoring chest pain — or stopping treatment early — can lead to problems that are much harder to manage. The risk of serious complications is low with proper care, but it rises sharply without it.
| Complication | Risk Level | What Happens |
|---|---|---|
| Recurrent Pericarditis | Moderate — 15–30% without colchicine | Inflammation returns weeks or months later |
| Pericardial Effusion | Common — up to 60% of cases | Fluid builds up around the heart; ranges from mild to severe |
| Cardiac Tamponade | Rare in viral cases (<2%); higher in bacterial | Too much fluid compresses the heart — life-threatening |
| Constrictive Pericarditis | Very rare (<1% in viral) | Scar tissue forms around the heart, restricting its movement |
| Myopericarditis | In some patients | Inflammation spreads to the heart muscle — needs close monitoring |
Completing your full course of colchicine is the single most important step to avoiding these complications.
9. How Can You Prevent Pericarditis From Coming Back?
You cannot always prevent the very first episode — especially when a virus is responsible. But preventing a second or third episode? That is largely within your control.
The single most important thing you can do is complete your full colchicine course — all 3 months of it, even when you feel completely fine. Most relapses happen because patients stop taking it early. Beyond that, rest until your doctor clears you for exercise, stay on top of any autoimmune conditions, treat infections early, and keep your follow-up appointments — your doctor will check CRP levels to confirm the inflammation is truly gone.
If you are scheduled for heart surgery, ask your doctor about colchicine prophylaxis beforehand — the guidelines now recommend it to prevent post-surgery pericarditis.
Finish your medicine. Rest properly. Stay consistent with follow-ups. That is the prevention plan — and it works.
10. When Should You See a Doctor?
Always see a doctor if you have unexplained chest pain. Never ignore it. Here is a simple guide:
| Situation | What to Do |
|---|---|
| Sharp chest pain that gets worse lying down | See a doctor the same day |
| Chest pain with fever or recent viral illness | Visit urgent care or ER |
| Chest pain with difficulty breathing or dizziness | Go to the nearest emergency room immediately |
| Known pericarditis — symptoms returning after treatment | Call your cardiologist promptly |
| Feeling better but want to resume exercise | Get clearance from your doctor first |
| New swelling of legs or abdomen | See your doctor — may indicate effusion |
11. Frequently Asked Questions (FAQ)
References & Sources
- Wang T, Klein A, Cremer P, et al. ACC Expert Consensus Statement on Diagnosis and Management of Pericarditis. J Am Coll Cardiol. 2025 Latest. doi:10.1016/j.jacc.2025.05.023
- Schulz-Menger J, et al. ESC Guidelines for the Management of Myocarditis and Pericarditis. Eur Heart J. 2025 Latest. ESC 2025
- Adler Y, et al. ESC Guidelines for the Diagnosis and Management of Pericardial Diseases. Eur Heart J. 2015. PMC7539677
- ESC Council for Cardiology Practice. Management of Acute Pericarditis: Treatment and Follow-up. 2024. escardio.org
- Myocarditis Foundation. Pericarditis Treatment: What’s New in the Latest Guidelines. 2025 Latest.
- National Institutes of Health (NIH) / MedlinePlus. Pericarditis. 2024. medlineplus.gov
- Mayo Clinic. Pericarditis — Symptoms & Causes. 2024. mayoclinic.org