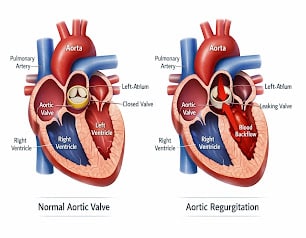
Aortic Regurgitation: The Silent Heart Condition Most People Don’t Know They Have
What You Will Learn in This Guide
- What is aortic regurgitation?
- How common is it worldwide?
- Early, silent, and emergency symptoms
- Causes and risk factors
- Types and disease stages
- How it damages the heart
- How it is diagnosed
- All treatment options
- Diet, exercise, and lifestyle
- Complications
- Life expectancy and prognosis
- When to see a doctor
- Research and expert references
- Patient FAQs
Introduction
Your heart beats around 100,000 times a day. Every single beat depends on four valves that open and close at exactly the right moment. When one of those valves stops working correctly, the consequences can quietly build for years before you ever feel anything at all.
Aortic regurgitation is exactly that kind of condition. It develops slowly, often without any warning. By the time most patients notice something is wrong — shortness of breath, fatigue, the heart pounding at night — the heart has already been compensating and straining for a long time.
I have been working in public health research and medical writing for over 15 years. In that time, I have reviewed hundreds of cardiology studies and worked with patients who received this diagnosis and had no idea what it really meant. This article is for them — and for anyone who wants to genuinely understand this condition, not just skim a list of symptoms.
What I want you to take away from this guide is not a list of scary facts. It is a clear understanding of what is happening inside the heart, what your options are, and what questions to ask your doctor. Aortic regurgitation is a manageable condition — but only when it is taken seriously.
What Is Aortic Regurgitation?
Aortic regurgitation (AR) — also known as aortic insufficiency — is a condition where the aortic valve does not close completely after each heartbeat. This incomplete closure allows blood to flow backward from the aorta into the left ventricle.
To understand this properly, you need to know where the aortic valve sits and what it is supposed to do.
The left ventricle is the heart’s main pumping chamber. After it fills with oxygenated blood coming from the lungs, it contracts and pushes that blood out through the aortic valve into the aorta — the body’s largest artery. The aortic valve then closes tightly to prevent any blood from returning. It is a one-way gate.
In aortic regurgitation, that gate does not seal properly. Blood flows the wrong way — back into the left ventricle. On the next beat, the ventricle now has to pump out its normal load of blood plus whatever has leaked back in. This is extra work it was never designed to do, and it does it every single beat, every single day.
Over time, this constant volume overload causes the left ventricle to enlarge — stretching its walls to accommodate more blood. For a while, this compensation works. Eventually, it does not. The walls weaken, the pumping function drops, and symptoms begin to appear.
How Common Is Aortic Regurgitation? Global Importance and Epidemiology
Aortic regurgitation is far more common than most people realize. Research published in the Journal of the American College of Cardiology estimates that moderate to severe AR affects approximately 0.5% of the general adult population — a figure that rises sharply after age 65.
The Global Burden of Disease study estimates that valvular heart diseases collectively affect over 100 million people worldwide. Among these, aortic regurgitation is the second most common valvular condition, after mitral regurgitation.
The cause of AR varies dramatically by geography. In low- and middle-income countries — including large parts of South Asia, Sub-Saharan Africa, and Latin America — rheumatic heart disease following untreated streptococcal throat infections remains the leading cause. In high-income countries, bicuspid aortic valve and age-related valve degeneration are responsible for the majority of cases.
This matters clinically. A 30-year-old in rural India with rheumatic AR and a 70-year-old in the United States with degenerative AR are dealing with fundamentally different diseases — even though the valve dysfunction looks the same on an echocardiogram.
What makes aortic regurgitation a significant public health challenge is its silent nature. A large proportion of patients live with moderate AR for years — sometimes a decade or more — without any symptoms. Many are diagnosed incidentally when an echocardiogram is ordered for an entirely different reason.
— AR affects approximately 0.5% of adults globally in moderate to severe form
— Prevalence increases to approximately 2% after age 70
— Up to 13% of elderly patients have at least mild AR on echocardiography
— Rheumatic heart disease causes 60–70% of AR cases in low-income countries
Aortic Regurgitation Symptoms
Early Symptoms
In the early stages of aortic regurgitation, most patients feel completely well. The heart is an extraordinarily adaptive organ. The left ventricle gradually expands to handle the extra blood volume, and for a surprisingly long time, this adaptation maintains normal function.
When early symptoms do appear, they tend to be subtle — easy to attribute to aging, stress, or simply being out of shape:
- Mild shortness of breath during strenuous physical activity — activities that never used to cause breathing difficulty
- A noticeable awareness of the heartbeat, particularly when lying on the left side at night
- Fatigue after moderate exertion that feels slightly out of proportion
- Occasional palpitations — a sense of the heart thumping, fluttering, or beating forcefully
- A faint, visible pulsation in the neck veins or chest wall in some patients
Silent Symptoms — What Patients Often Miss
Here is the most important thing I want every reader to understand about aortic regurgitation: the absence of symptoms is not the same as the absence of disease.
The heart compensates so well — for so long — that patients can have significant valve leakage, a noticeably enlarged left ventricle, and impaired pumping function while still feeling essentially normal day to day. Cardiologists call this the asymptomatic phase. It can last for years, sometimes decades.
During this phase, the only way to know what is happening is through regular echocardiograms. There is no symptom, no feeling, no warning sign that reliably tells you whether the heart is holding steady or slowly deteriorating underneath the surface.
This is precisely why routine cardiac evaluation matters. A heart murmur picked up during a routine physical exam — or even during a visit for something entirely unrelated — is often the first and only clue that aortic regurgitation is present.
Severe and Emergency Symptoms
When the left ventricle can no longer compensate, the clinical picture changes rapidly. This transition from asymptomatic to symptomatic marks a critical turning point — and at this stage, surgery can no longer be deferred.
- Significant shortness of breath even at rest, or when lying flat in bed (orthopnea)
- Waking up suddenly at night unable to breathe — gasping for air (paroxysmal nocturnal dyspnea)
- Chest pain or angina, particularly with physical activity
- Severe, crushing fatigue with dramatically reduced exercise tolerance
- Swollen legs, ankles, and feet from fluid retention (peripheral edema)
- Rapid, irregular, or forceful heartbeat
- Dizziness or episodes of near-fainting
Unlike chronic AR, which develops gradually, acute aortic regurgitation is sudden and life-threatening. It most commonly results from infective endocarditis or aortic dissection. Symptoms include sudden severe breathlessness, chest pain, low blood pressure, cold clammy skin, and cardiovascular collapse. Call emergency services immediately. This is not a condition that can wait for a scheduled appointment.
Causes of Aortic Regurgitation
AR can result from structural problems with the valve leaflets themselves, or from dilation of the aortic root — the section of the aorta where the valve is anchored. When the root dilates, it pulls the leaflet attachment points apart, preventing proper closure even if the leaflets themselves are structurally normal.
Primary Valve Causes
- Bicuspid aortic valve — the most common congenital heart defect, present in 1–2% of the general population. The valve has two leaflets instead of the normal three, making it structurally prone to regurgitation over decades. The most common cause in younger patients in high-income countries.
- Rheumatic heart disease — follows untreated Group A streptococcal throat infections. The inflammatory process scars and thickens the valve leaflets, causing them to retract and fail to close. Still accounts for the majority of AR cases in lower-income regions.
- Infective endocarditis — bacterial infection of the valve can rapidly destroy leaflet tissue, causing sudden and severe regurgitation. One of the main causes of acute AR.
- Degenerative valve disease — age-related calcification and fibrosis of the valve, increasingly seen after 65. The valve becomes stiff, irregular, and unable to seal properly.
- Autoimmune diseases — systemic lupus erythematosus, ankylosing spondylitis, and rheumatoid arthritis can all cause valve inflammation and secondary regurgitation.
Aortic Root Causes
- Marfan syndrome — a connective tissue disorder causing progressive aortic root dilation and AR, often presenting in young adults.
- Chronic hypertension — sustained high blood pressure gradually enlarges the aortic root over years.
- Aortic aneurysm — abnormal dilation of the aorta stretches the valve annulus.
- Aortic dissection — a tear in the aortic wall can acutely disrupt valve support structures, causing sudden severe AR.
Risk Factors
- Age over 65 — degenerative valve disease increases with age
- Male sex — AR is significantly more common in men
- History of rheumatic fever or recurrent untreated strep throat infections
- Known congenital bicuspid aortic valve
- Chronic, poorly controlled high blood pressure
- Connective tissue disorders — Marfan syndrome, Ehlers-Danlos syndrome
- Family history of bicuspid aortic valve or aortic root disease
- History of intravenous drug use — major risk factor for infective endocarditis
- Prior radiation therapy to the chest
- Certain autoimmune conditions — lupus, ankylosing spondylitis
Types of Aortic Regurgitation and Disease Progression
Chronic Aortic Regurgitation
Develops gradually over months to years. The left ventricle adapts by expanding its cavity — a process cardiologists call eccentric hypertrophy. This maintains cardiac output for a prolonged period. Most patients remain asymptomatic for years. However, left untreated, the ventricle eventually reaches the limits of compensation and function begins to deteriorate.
Acute Aortic Regurgitation
Occurs suddenly — most often due to infective endocarditis, aortic dissection, or chest trauma. The normal-sized left ventricle has no time to adapt to the sudden volume overload. The result is acute pulmonary edema and cardiovascular collapse. This is always a surgical emergency.
Severity Stages
| Stage | Valve Finding | LV Response | Symptoms | Action |
|---|---|---|---|---|
| Mild AR | Small regurgitant jet | Normal | None | Echo every 3–5 years |
| Moderate AR | Moderate jet, mild LV dilation | Early enlargement | Possibly exertional | Echo every 1–2 years |
| Severe AR (asymptomatic) | Large jet, significant dilation | Significant enlargement | None yet | Echo every 6–12 months |
| Severe AR (symptomatic) | Large jet, LV dysfunction | Dilated, weakened | Dyspnea, angina, HF | Surgery indicated |
How Aortic Regurgitation Damages the Heart
Understanding the mechanism helps explain why the timing of treatment is so critical.
With each heartbeat, the leaking valve allows a portion of ejected blood to return to the left ventricle. The ventricle now handles both its normal filling from the left atrium and the returning regurgitant blood. Total volume per beat increases — this is called volume overload.
To compensate, the left ventricle dilates — its walls stretch outward to accommodate more volume. For a period, the ejection fraction remains normal because the ventricle has simply grown larger. The patient feels fine.
But the stretched walls now generate higher wall stress. To normalize this stress, the heart adds muscle mass through hypertrophy. The ventricle becomes both dilated and hypertrophied — a combination that eventually impairs its ability to relax properly between beats.
Over years, the sustained overload leads to myocardial fibrosis — permanent scarring of the heart muscle. Once significant fibrosis develops, surgical repair may improve symptoms but cannot fully restore normal LV function. This is why surgery before irreversible damage occurs is so important.
How Is Aortic Regurgitation Diagnosed?
Diagnosis begins at the bedside. An experienced cardiologist can detect the characteristic murmur of AR with a stethoscope — a high-pitched, blowing diastolic sound heard best along the left sternal border when the patient leans forward and exhales. However, clinical examination alone cannot determine severity or quantify the impact on the heart. Imaging is essential.
Echocardiogram — The Gold Standard
The transthoracic echocardiogram (TTE) is the cornerstone of AR assessment. It provides direct visualization of the valve, color Doppler quantification of the regurgitant jet, measurement of left ventricular dimensions, assessment of ejection fraction, and evaluation of the aortic root.
Transesophageal Echocardiogram (TEE)
A probe passed into the esophagus provides higher resolution imaging. Used when TTE is technically limited, when infective endocarditis is suspected, or for detailed preoperative planning.
Cardiac MRI
Currently the most accurate method for quantifying regurgitant volume and assessing LV function. Particularly valuable in cases where echocardiographic measurements are borderline or inconsistent with symptoms.
Other Diagnostic Tests
- Chest X-ray — may show an enlarged heart and pulmonary congestion in advanced AR
- ECG — ECG can reveal LV hypertrophy or rhythm disturbances
- Exercise stress testing — sometimes used to unmask effort-induced symptoms in asymptomatic severe AR
- Cardiac catheterization — used preoperatively in older patients to evaluate coronary artery disease simultaneously
Aortic Regurgitation Treatment Options
1. Watchful Waiting — Structured Monitoring
For mild to moderate AR without symptoms, careful surveillance is appropriate and evidence-based. This is not passive neglect — it is a structured protocol of regular echocardiographic monitoring to catch any progression before it becomes irreversible.
- Mild AR: echocardiogram every 3–5 years
- Moderate AR: echocardiogram every 1–2 years
- Severe asymptomatic AR: echocardiogram every 6–12 months with close clinical review
2. Medications
No medication can close a leaking valve or stop AR from progressing. Medications manage the consequences of volume overload and reduce cardiovascular risk while monitoring continues or surgery is being planned.
- ACE inhibitors or ARBs — reduce blood pressure and afterload. First choice for symptomatic patients and for patients with hypertension and AR.
- Beta-blockers — used cautiously; helpful for hypertension management and rate control in associated atrial fibrillation.
- Diuretics — reduce fluid retention in patients with heart failure symptoms. Improve breathlessness and edema.
- Antibiotic prophylaxis — recommended before certain high-risk dental procedures in patients with prior valve surgery, rheumatic heart disease, or endocarditis history.
3. Surgery — The Definitive Treatment
Surgery is the only treatment that directly addresses the valve problem. According to the 2021 ACC/AHA guidelines, valve surgery is indicated in severe AR when any of the following are present:
- Development of symptoms — dyspnea, angina, or heart failure
- Left ventricular ejection fraction falls below 55%
- LV end-systolic diameter exceeds 50 mm
- Undergoing cardiac surgery for another indication simultaneously
Surgical Options
Aortic Valve Replacement (AVR) — the gold standard. The damaged valve is replaced with either a mechanical valve (extremely durable, requires lifelong anticoagulation with warfarin, preferred in younger patients) or a biological tissue valve (no anticoagulation needed, may require re-intervention after 15–20 years, preferred in older patients).
Valve Repair — preserving the patient’s own valve rather than replacing it. Avoids prosthetic valve complications. Technically demanding and only possible in select patients with favorable anatomy. Best outcomes at experienced high-volume centers.
TAVR (Transcatheter Aortic Valve Replacement) — a minimally invasive, catheter-based approach. Currently primarily used in high surgical risk patients. Its role in AR continues to evolve with new dedicated device designs in clinical trials.
4. Advanced Treatments Under Development
Research is actively ongoing into dedicated transcatheter devices for AR, robotic-assisted valve repair, and bioengineered tissue valves with greater long-term durability. Several major cardiac centers are enrolling patients in trials evaluating next-generation devices specifically designed for the anatomical challenges of AR.
Lifestyle, Diet, and Prevention
Diet Recommendations for Aortic Regurgitation
Diet cannot repair a leaking valve. But the right nutritional choices meaningfully reduce blood pressure, protect heart muscle function, reduce systemic inflammation, and slow the progression of associated cardiovascular risk. This is a core part of disease management, not optional.
What to Eat More Of
- Fruits and vegetables — aim for five or more portions daily. Potassium-rich options like bananas, sweet potatoes, spinach, and avocado help lower blood pressure naturally.
- Whole grains — oats, brown rice, quinoa, whole wheat. Reduce LDL cholesterol and provide sustained energy.
- Fatty fish — salmon, mackerel, sardines, trout. Two to three portions per week provide omega-3 fatty acids that reduce inflammation and protect cardiac function.
- Legumes and beans — excellent fiber, plant protein, and potassium. Lentils, chickpeas, kidney beans.
- Olive oil — primary cooking fat. Anti-inflammatory and heart-protective.
- Nuts and seeds — walnuts, flaxseeds, chia seeds in moderate amounts.
What to Reduce or Avoid
- High-sodium foods — sodium drives fluid retention and elevates blood pressure, both of which worsen AR. Target under 1500–2000 mg per day. Watch hidden sodium in processed foods, canned soups, and restaurant meals.
- Saturated and trans fats — processed meats, fried foods, packaged snacks. Contribute to atherosclerosis and hypertension.
- Alcohol — directly suppresses myocardial contractility and worsens left ventricular function. Limit strictly or eliminate.
- Excessive caffeine — can trigger palpitations in sensitive individuals.
- Sugary beverages and ultra-processed foods — contribute to obesity, metabolic syndrome, and hypertension.
Exercise Guidelines
- Mild to moderate AR — moderate aerobic exercise is safe and encouraged. Walking, cycling, swimming, and light jogging. Aim for 150 minutes per week.
- Severe asymptomatic AR — low to moderate aerobic activity is generally acceptable. Avoid competitive sports. Discuss your specific program with your cardiologist.
- Severe symptomatic AR or post-surgery — exercise should be supervised and individualized. Formal cardiac rehabilitation programs are strongly recommended after valve surgery.
- Avoid for severe AR — heavy weightlifting, high-intensity isometric exercise, contact sports, and competitive athletics without explicit specialist clearance.
Prevention Tips
- Treat strep throat promptly and completely — this prevents rheumatic fever, the leading preventable cause of AR globally
- Monitor and control blood pressure consistently
- Maintain excellent dental hygiene to reduce endocarditis risk
- Avoid intravenous drug use — a primary risk factor for endocarditis-related valve destruction
- If you have a known bicuspid valve or family history of connective tissue disorders — undergo regular cardiac screening even without symptoms
Genetic and Family History Considerations
Bicuspid aortic valve — the most common congenital cause of AR — has a clear hereditary component. First-degree relatives of patients with a bicuspid valve have a 10–15 times higher risk of also having one. Current guidelines recommend echocardiographic screening of first-degree relatives when a bicuspid valve is confirmed.
Connective tissue disorders such as Marfan syndrome (FBN1 gene) and Loeys-Dietz syndrome have autosomal dominant inheritance patterns. Genetic counseling and family screening are recommended when these diagnoses are confirmed.
Aortic Regurgitation vs. Aortic Stenosis — What Is the Difference?
| Feature | Aortic Regurgitation | Aortic Stenosis |
|---|---|---|
| Problem | Valve does not close fully | Valve does not open fully |
| Blood flow | Backward leak into LV | Restricted forward flow |
| Effect on heart | Volume overload of LV | Pressure overload of LV |
| LV response | Dilation (eccentric hypertrophy) | Wall thickening (concentric hypertrophy) |
| Pulse | Wide, bounding pulse | Narrow, weak pulse |
| Common in | Younger adults, bicuspid valve, rheumatic disease | Older adults, calcific degeneration |
| Treatment | AVR or valve repair | AVR or TAVR |
Both conditions can coexist in the same patient — called mixed aortic valve disease — and both may ultimately require surgical intervention.
Complications of Aortic Regurgitation
- Heart failure — the most common and serious complication. Progressive LV dysfunction eventually leads to reduced cardiac output and congestion.
- Atrial fibrillation — irregular heart rhythm from elevated pressures in cardiac chambers. Increases stroke risk.
- Infective endocarditis — abnormal or previously damaged valves are significantly more susceptible to bacterial infection.
- Sudden cardiac death — rare but documented in patients with severe untreated AR, particularly during strenuous exertion.
- Aortic dissection — particularly relevant in patients with underlying aortic root dilation from Marfan syndrome or bicuspid valve disease.
- Irreversible LV dysfunction — if severe AR is allowed to progress too long without surgery, the left ventricle may not fully recover its function even after valve replacement.
Prognosis and Life Expectancy
The prognosis of aortic regurgitation is closely tied to three factors: severity, timing of surgical intervention, and baseline left ventricular function at the time of surgery.
Without Surgery
- Mild AR — normal life expectancy. Most patients never progress to severe disease. Regular monitoring is sufficient.
- Moderate AR (asymptomatic) — approximately 3–4% of patients per year progress to requiring surgery. Most live for many years without significant problems with appropriate monitoring.
- Severe AR (asymptomatic) — progression to symptoms or LV dysfunction occurs at approximately 4–6% per year. Close surveillance is essential.
- Severe AR (symptomatic, untreated) — mortality is approximately 10% per year once angina or heart failure develops. Symptom onset is a clear surgical trigger.
After Successful Valve Surgery
Outcomes after aortic valve replacement for AR are generally excellent when surgery is performed before irreversible LV damage. Ten-year survival post-surgery exceeds 70–80% in major surgical series — approaching age-matched population norms.
A landmark study by Dujardin KS, Enriquez-Sarano M, and colleagues, published in Circulation (1999), established that the onset of symptoms in severe AR is the single most important prognostic threshold. Asymptomatic patients with preserved LV function had significantly better long-term outcomes, reinforcing the rationale for proactive surgical timing before symptoms emerge.
When to See a Doctor — Patient Awareness and Warning Signs
Schedule an Appointment if You Notice:
- New or worsening shortness of breath with activities you used to manage easily
- Unexplained fatigue or a decline in your usual exercise tolerance
- Palpitations — a feeling of the heart pounding, racing, or skipping beats
- Swelling in your legs, ankles, or feet that is new
- Any chest discomfort or heaviness
- You have been told you have a heart murmur and have never had an echocardiogram
— Sudden, severe breathlessness that comes on rapidly
— Chest pain at rest, especially if new or severe
— Dizziness, fainting, or near-fainting
— Cold, clammy skin with a rapid weak pulse
— Confusion or sudden extreme weakness
These may indicate acute aortic regurgitation or decompensated heart failure — both are life-threatening emergencies.
Key Warning Signs Patients Often Ignore
- Sleeping with more pillows than usual to breathe comfortably — this is orthopnea, a sign of early heart failure
- Waking up breathless at 2–3 AM needing to sit up — paroxysmal nocturnal dyspnea
- Noticing the neck arteries visibly pulsating — a sign of wide pulse pressure in significant AR
- Feeling the heart thumping strongly in the chest at rest — a sign of hyperdynamic circulation from volume overload
Screening Guidelines
- First-degree relatives of patients with bicuspid aortic valve — one-time echocardiogram recommended
- Patients with Marfan syndrome or other connective tissue disorders — regular echocardiographic surveillance
- Patients with a history of rheumatic fever — echocardiogram to evaluate valve involvement
- Patients with known heart murmur — echocardiogram to classify type and severity
- Patients with unexplained dyspnea or reduced exercise tolerance — echocardiogram as part of initial workup
Recovery After Aortic Valve Surgery
- Hospital stay — usually 5–7 days for uncomplicated cases
- Breastbone healing — 6–8 weeks. Lifting and strenuous arm activity restricted during this period.
- Return to light activity — most patients walk independently within 2–4 weeks
- Return to driving — typically 4–6 weeks when cleared by the surgeon
- Return to work — desk work: 4–6 weeks; physical labor: 3–4 months or longer
- Full recovery — 3–6 months for most patients
- Cardiac rehabilitation — strongly recommended; supervised exercise beginning 4–6 weeks post-surgery significantly improves outcomes
Long-Term Management of Chronic Aortic Regurgitation
- Regular echocardiograms — non-negotiable. Mild: every 3–5 years. Moderate: every 1–2 years. Severe: every 6–12 months.
- Blood pressure control — target below 130/80 mmHg. Consistently elevated BP accelerates valve and root damage.
- Medication adherence — take all prescribed medications without interruption.
- Dental hygiene — inform your dentist of your valve condition at every appointment.
- Symptom diary — tracking daily symptoms and exercise tolerance helps detect subtle deterioration between appointments.
- Mental health support — anxiety and health-related worry are common in patients with chronic cardiac conditions and deserve attention.
- Annual primary care review — in addition to cardiology follow-up, for overall cardiovascular risk management.
Latest Medical Research and Global Health Insights
- Dedicated TAVR devices for AR — unlike aortic stenosis where TAVR is now standard, AR presents unique anatomical challenges. New dedicated catheter-based designs are in clinical trials.
- Biomarkers for surgical timing — researchers are investigating whether BNP and NT-proBNP can help identify asymptomatic patients approaching the surgical threshold before LV dysfunction becomes overt.
- AI-assisted echocardiography — machine learning algorithms are being validated to improve consistency in AR quantification across different imaging centers.
- WHO Global Heart Initiative — the World Health Organization continues to push for improved access to echocardiography in low-income countries, where undiagnosed rheumatic AR remains a major cause of preventable cardiac death in young people.
Research Studies, Expert Opinions and Medical References
- Otto CM, Nishimura RA, Bonow RO, et al. — 2021 ACC/AHA Guideline for the Management of Patients With Valvular Heart Disease. Journal of the American College of Cardiology, 2021. The current evidence-based clinical framework for AR management and surgical timing.
- Dujardin KS, Enriquez-Sarano M, Schaff HV, et al. — Mortality and Morbidity of Aortic Regurgitation in Clinical Practice: A Long-Term Follow-Up Study. Circulation, 1999. Established symptom onset as the critical prognostic threshold in severe AR.
- Braunwald’s Heart Disease: A Textbook of Cardiovascular Medicine — Libby P, Bonow RO, Mann DL, et al. (Eds). The definitive medical reference for cardiovascular disease management.
- Lancellotti P, Tribouilloy C, Hagendorff A, et al. — Recommendations for the Echocardiographic Assessment of Native Valvular Regurgitation. European Journal of Echocardiography, 2013.
- World Heart Federation — Global epidemiological data on the burden of valvular and rheumatic heart disease worldwide.
- Dr. Robert O. Bonow — former President of the American Heart Association, professor of cardiology at Northwestern University, and leading authority on the natural history and surgical timing of valvular heart disease.
- GBD 2019 Diseases and Injuries Collaborators — Global Burden of Disease Study 2019. The Lancet, 2020. Source of global valvular disease prevalence data.
Patient Frequently Asked Questions
It means your aortic heart valve is leaking. Instead of closing properly after each heartbeat, it lets blood flow backward into the heart. Over time, this forces the heart to work much harder than it should — and without treatment, that extra work damages the heart muscle.
No. Medications help manage symptoms and protect the heart, but they cannot close a leaking valve or stop the disease from progressing. Aortic valve replacement or repair is the only treatment that directly fixes the problem in significant AR. Outcomes after surgery are generally excellent when it is done at the right time.
Mild AR is generally not immediately dangerous. Most patients with mild AR live normally for many years without the condition progressing significantly. The key is not to ignore it. Regular echocardiograms are important to catch any change early.
Stenosis means the valve does not open fully — blood flow out of the heart is restricted. Regurgitation means the valve does not close fully — blood leaks backward. Same valve, opposite problems. Stenosis creates pressure overload. Regurgitation creates volume overload. Both can eventually require surgery.
Avoid high-sodium foods, saturated and trans fats, excessive alcohol, and anything that consistently triggers palpitations. Focus on vegetables, whole grains, lean proteins, fatty fish, and heart-healthy fats like olive oil. A heart-healthy diet cannot fix the valve, but it meaningfully reduces blood pressure and cardiovascular strain.
Yes — moderate aerobic exercise is generally safe and beneficial for mild to moderate AR. Walking, cycling, swimming, and light jogging are appropriate. If you have severe AR, avoid competitive sports and heavy weightlifting. Always discuss your specific exercise program with your cardiologist before making significant changes.
Some causes have a clear genetic component. Bicuspid aortic valve runs in families — first-degree relatives of affected patients have a 10–15 times higher risk. Connective tissue disorders like Marfan syndrome are inherited in an autosomal dominant pattern. If a close relative has a bicuspid valve or aortic disease, ask your doctor about echocardiographic screening.
Untreated severe AR leads to progressive left ventricular enlargement and dysfunction, culminating in heart failure. Once symptoms appear, mortality without surgery is approximately 10% per year. If surgery is delayed too long, the left ventricle may not fully recover its function even after a successful valve replacement. Early intervention is the most important factor in long-term outcome.
With mild AR and no symptoms — normal life expectancy with monitoring. With severe AR treated by timely surgery — most patients return to near-normal life expectancy. The key variable is whether surgery happens before the left ventricle loses its ability to recover. Untreated severe symptomatic AR carries mortality of roughly 10% per year.
In early stages, most patients feel nothing at all. When symptoms do appear, the most common descriptions are: a sense of the heart pounding or thumping forcefully — especially when lying down at night — shortness of breath with activities that never caused it before, and fatigue that feels disproportionate to the effort. Some patients describe an uncomfortable awareness of their own heartbeat.
Author: Iraphan Khan — Public Health Researcher and Medical Content Writer at RealMedVision