Angina — Chest Pain
What It Means, Types, Causes, How Doctors Check It, Treatment & When to Go to Hospital
Introduction
Chest pain is one of the most frightening sensations a person can experience. And one of the most common mistakes people make when it happens is finding a reason to dismiss it. Gas. Acidity. Muscle pull. Stress. These explanations feel reassuring — and sometimes they are correct. But sometimes they are not. And the cases where the pain was actually coming from the heart, and was ignored for weeks or months before something serious happened, are far more common than most people realize.
Angina is chest pain or discomfort that occurs when the heart muscle is not receiving enough blood — and therefore not enough oxygen — to meet its demands. It is not a heart attack. No permanent damage has occurred yet. But it is the heart’s way of signaling that the blood supply is becoming insufficient, and that the underlying condition causing it needs attention before something more serious develops.
The American Heart Association first formally described angina as a clinical syndrome distinct from heart attack in its cardiovascular guidelines in the mid-20th century, and research since then has consistently reinforced its significance as a warning sign. The World Health Organization, in its 2021 global cardiovascular disease report, identified angina as one of the most important clinical presentations of coronary artery disease — the leading cause of death worldwide. In India, AIIMS researchers have documented in multiple studies from the 2000s and 2010s that a significant number of patients who present with their first heart attack had experienced prior episodes of chest discomfort that they had attributed to non-cardiac causes and had not investigated.
As a medical researcher, I have reviewed data from WHO, AHA, AIIMS, and peer-reviewed cardiology literature to put this guide together. Understanding angina — what it feels like, what causes it, and when it demands immediate attention — can genuinely prevent a heart attack.
What Does Angina Mean?
Angina is chest pain or pressure that occurs when the blood supply to the heart muscle becomes temporarily insufficient. The heart is a continuously working muscle — it beats roughly 100,000 times a day — and it requires a constant, uninterrupted supply of oxygen-rich blood to do this. That blood is delivered through the coronary arteries.
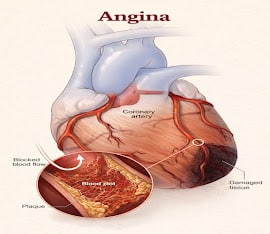
When these arteries are healthy and open, blood flows freely and the heart receives all the oxygen it needs. When the arteries become narrowed — due to plaque buildup from cholesterol and fat deposits along the artery walls — the blood flow becomes restricted. At rest, this restriction may be manageable. But during physical activity or emotional stress, when the heart’s demand for oxygen increases, the narrowed arteries cannot keep up. The result is a temporary oxygen shortage in the heart muscle — and that shortage is felt as chest pain or pressure.
Importantly, in angina, this process is temporary and reversible. Rest or medication restores the balance between supply and demand, and the pain passes. This is what distinguishes angina from a heart attack — in which the blockage is complete and permanent damage to the heart muscle occurs.
How Does Angina Feel?
One of the reasons angina is so often missed or misattributed is that it does not always feel the way people expect chest pain to feel. It is not always a sharp, stabbing pain. More commonly, patients describe it as a pressure, a tightness, a squeezing or heaviness in the chest — as though something heavy is sitting on it, or a band is tightening around it.
The discomfort may stay localized in the chest, or it may radiate — spreading to the left arm, the neck, the jaw, the shoulder, or the upper back. This radiation pattern, which results from the way heart pain signals travel through shared nerve pathways, is one of the most diagnostically important features of cardiac chest pain.
Other symptoms that may accompany angina include shortness of breath, sweating, nausea, and dizziness. In women and older patients — a pattern recognized in AHA research from the early 2000s — the presentation is often atypical. Strong chest pressure may be absent entirely, with the predominant symptoms being unusual fatigue, breathlessness, jaw or back discomfort, or a vague sense that something is wrong. This atypical presentation is one reason why angina in women is sometimes diagnosed later than in men.
Types of Angina
1. Stable Angina
This is the most common form. Stable angina follows a predictable pattern — it comes on with physical exertion or emotional stress, and resolves within a few minutes of rest or after taking nitroglycerine. The consistency of this pattern is actually reassuring in one sense — it means the condition is predictable and can be managed. However, it still requires medical evaluation and treatment, because it indicates significant underlying coronary artery disease.
2. Unstable Angina
Unstable angina is a medical emergency. In this form, the pattern changes — pain may occur at rest, last longer than usual, be more severe, or appear with less provocation than before. It signals that the situation inside the coronary arteries has changed — a plaque may have become unstable or partially ruptured, making a complete blockage and heart attack much more likely in the hours and days that follow. Anyone with new or changing chest pain should seek emergency evaluation without delay.
3. Variant Angina
Also called Prinzmetal angina, this type occurs when a coronary artery goes into a sudden, temporary spasm — squeezing tightly and cutting off blood flow for a short time. It is not caused by fixed plaque buildup in the artery, and it often occurs at rest, typically at night or in the early morning hours. It can be associated with smoking, stress, cocaine use, or certain medicines. Though less common than stable angina, it can produce severe, alarming symptoms and requires specific treatment.
4. Microvascular Angina
This form involves dysfunction in the very small blood vessels — the microvasculature — of the heart, rather than the large coronary arteries. It is seen more commonly in women, and it presents a diagnostic challenge because standard tests like stress testing and angiography often appear normal. AIIMS researchers have highlighted microvascular angina as an underdiagnosed condition in Indian women, contributing to cases where patients are told their heart is fine when they are genuinely experiencing cardiac chest pain.
Why Does Angina Happen
The underlying cause of most angina is coronary artery disease — the gradual narrowing of the heart’s blood vessels due to plaque buildup. And the drivers of coronary artery disease are well-established and largely modifiable. According to the American Heart Association’s 2019 Heart Disease and Stroke Statistics report, the major contributors include high blood pressure, which damages artery walls over time; high LDL cholesterol, which deposits into those damaged walls; diabetes, which accelerates arterial damage through multiple mechanisms; smoking, which both injures the arterial lining and promotes clotting; obesity; and physical inactivity.
Emotional stress deserves specific mention. Acute psychological stress causes the release of adrenaline, which raises heart rate and blood pressure — increasing the heart’s oxygen demand suddenly. In a person with already narrowed arteries, this spike in demand can be enough to trigger an angina episode even without physical exertion. This is why angina sometimes appears to follow an argument, a difficult conversation, or a sudden shock.
Who Has Higher Risk?
The risk of developing angina is significantly higher in people who have one or more of the following: a family history of coronary artery disease or early heart attack in a first-degree relative, high blood pressure, diabetes, elevated LDL cholesterol, overweight or obesity, a smoking habit, low physical activity, or chronic psychological stress. In India, ICMR data has shown that the combination of diabetes and hypertension — which is increasingly common — carries a particularly high risk of premature coronary artery disease and angina.
How Doctors Check Angina
When a patient presents with chest pain, the cardiologist takes a detailed history — asking about the character of the pain, when it occurs, how long it lasts, what brings it on, and what makes it better. This clinical history alone provides enormous diagnostic information. Tests are then used to confirm the diagnosis, assess severity, and guide treatment.
- ECG — may show changes during an angina episode, and can reveal evidence of previous silent heart attacks
- Stress test — Treadmill Test — the patient exercises on a treadmill while being monitored with an ECG. Changes in heart activity during exertion help confirm whether the coronary blood supply is adequate
- Blood tests — to check cholesterol, blood sugar, and cardiac biomarkers
- Echocardiogram — shows heart structure, valve function, and pumping strength
- Coronary angiography — the definitive test for visualizing blockages inside the coronary arteries. A thin catheter is guided to the heart and contrast dye is injected to reveal the arteries on X-ray imaging
How Is Angina Treated?
Treatment in angina has three goals — relieve symptoms, prevent heart attacks, and slow the progression of the underlying coronary artery disease. The approach combines medicines, lifestyle changes, and in some cases, procedures to open blocked arteries.
Medicines
Several medicines are used in angina management. Nitrates — including short-acting nitroglycerine — rapidly relieve acute angina episodes by dilating blood vessels and reducing the heart’s workload. Beta blockers and calcium channel blockers reduce heart rate and blood pressure, decreasing the heart’s oxygen demand. Antiplatelet medicines like aspirin prevent blood clots from forming on plaques. Statins lower LDL cholesterol and stabilize plaques, reducing the risk of rupture. All medicines must be taken consistently as prescribed — stopping them without medical advice can be dangerous.
Lifestyle Changes
Lifestyle changes are not supplementary to angina treatment — they are central to it. Stopping smoking produces immediate cardiovascular benefits. A diet low in saturated fat, salt, and processed foods, combined with regular aerobic exercise, reduces blood pressure, cholesterol, and body weight simultaneously. Stress management — through regular physical activity, adequate sleep, and relaxation techniques — reduces the frequency of stress-triggered episodes. These changes, consistently maintained, slow the progression of coronary artery disease in a way that medicines alone cannot fully replicate.
Medical Procedures
When arteries are severely narrowed and symptoms are not adequately controlled with medicines, interventional treatment may be needed. Percutaneous coronary intervention — commonly called coronary angioplasty or stenting — involves passing a thin tube into the blocked artery and inflating a small balloon to open it, then leaving a metal stent in place to keep it open. Coronary artery bypass surgery creates new pathways for blood to reach the heart, bypassing the blocked segments. The decision between these options depends on the pattern and severity of the blockages and the patient’s overall condition.
How To Prevent Angina
The majority of angina cases are preventable — because the coronary artery disease that causes them is preventable. The steps are consistent with overall cardiovascular health: stay physically active, eat a balanced diet low in saturated fat and salt, control blood pressure and blood sugar, avoid tobacco entirely, manage stress, and attend regular health checkups. The WHO’s 2021 report emphasized that at least 80 percent of premature cardiovascular disease — including angina and heart attack — is preventable through these modifiable lifestyle factors.
When To Go To Hospital Fast
Go to the emergency department immediately if:
• Chest pain or pressure lasts more than a few minutes and does not pass with rest
• Pain occurs at rest — especially if this is new or different from before
• The pain is unusually severe or feels different from previous episodes
• Chest pain is accompanied by sweating, nausea, vomiting, or fainting
• You feel sudden weakness, difficulty speaking, or vision changes alongside chest pain
These symptoms may indicate unstable angina or an evolving heart attack. Every minute of delay increases the risk of permanent heart muscle damage. Do not drive yourself — call for emergency help immediately.
• Chest pain or pressure lasts more than a few minutes and does not pass with rest
• Pain occurs at rest — especially if this is new or different from before
• The pain is unusually severe or feels different from previous episodes
• Chest pain is accompanied by sweating, nausea, vomiting, or fainting
• You feel sudden weakness, difficulty speaking, or vision changes alongside chest pain
These symptoms may indicate unstable angina or an evolving heart attack. Every minute of delay increases the risk of permanent heart muscle damage. Do not drive yourself — call for emergency help immediately.
Frequently Asked Questions (FAQ)
Is angina a heart attack?
No. Angina is temporary chest pain — no permanent damage. A heart attack is a complete blockage that destroys heart muscle. But unstable angina is serious and can quickly turn into a heart attack. Never ignore new or changing chest pain.
How long does the pain last?
Usually 2 to 5 minutes with rest or medicine. If pain lasts more than 10 to 15 minutes and does not go away — go to emergency immediately.
Can angina be managed long term?
Yes. With the right medicines, lifestyle changes, and regular follow-up, many people live normal active lives. The key is not ignoring any change in symptoms
Medical Disclaimer
This article is written for general educational awareness only. It does not constitute medical advice, diagnosis, or treatment recommendation. If you experience chest pain — particularly new, severe, or changing chest pain — please consult a qualified cardiologist or seek emergency care without delay.
This article is written for general educational awareness only. It does not constitute medical advice, diagnosis, or treatment recommendation. If you experience chest pain — particularly new, severe, or changing chest pain — please consult a qualified cardiologist or seek emergency care without delay.



.jpg)
.jpg)