Ejection Fraction (EF)
What Ejection Fraction Means and Why It Matters
A patient-friendly guide by RealMedVision
Last Update – May 2026
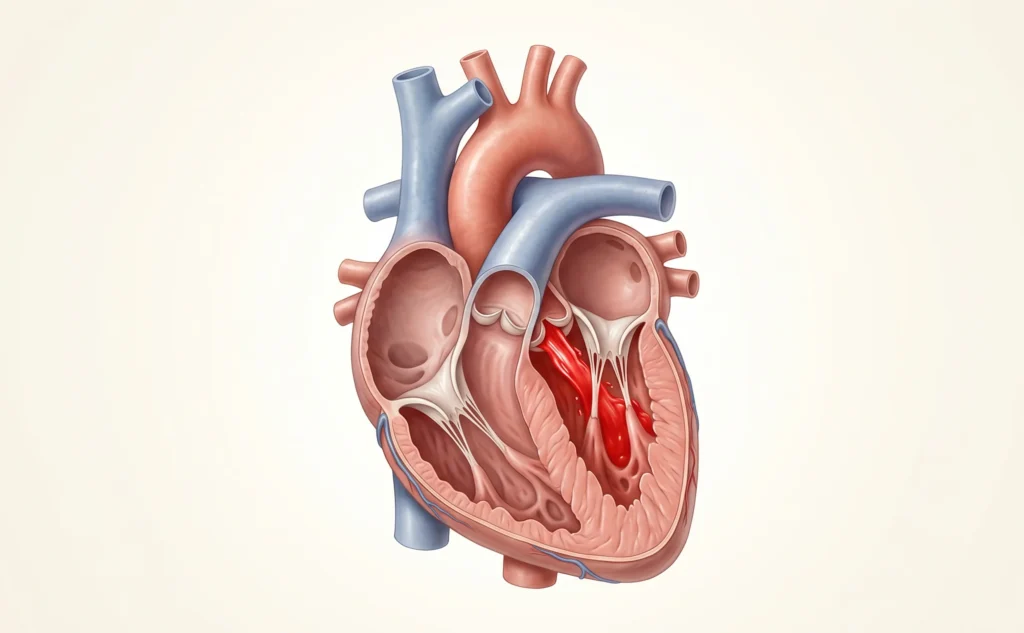
Ejection Fraction normal range is something that tells you how well your heart is pumping. Most people only hear about it when their report says “EF 40%” or “EF reduced” and that moment of confusion or worry is completely understandable.
Simply put Ejection Fraction is a percentage that shows how much blood your heart pushes out with each beat.
The Ejection Fraction normal range is usually between 55% and 70%. This means a healthy heart pushes out more than half the blood it holds every time it beats helping your body get the oxygen it needs.
When this number falls below 55% especially if it drops close to 40% or lower it means the heart is not pumping as strongly as it should.
In this guide we’ll break down what your number means why it drops and what steps can actually help improve it.
What We Will Cover in This Article
- What Ejection Fraction (EF) actually means — in simple, plain language
- What is considered a normal EF range
- What low EF and high EF indicate about your heart
- How EF is linked to heart failure
- Common symptoms when EF is reduced
- How doctors measure EF (tests like echocardiography)
- Whether EF can improve — and how
- Simple steps to protect your heart and maintain EF
- When you should get your EF checked
What Is Ejection Fraction?
Let me explain this with an analogy that makes it immediately clear.
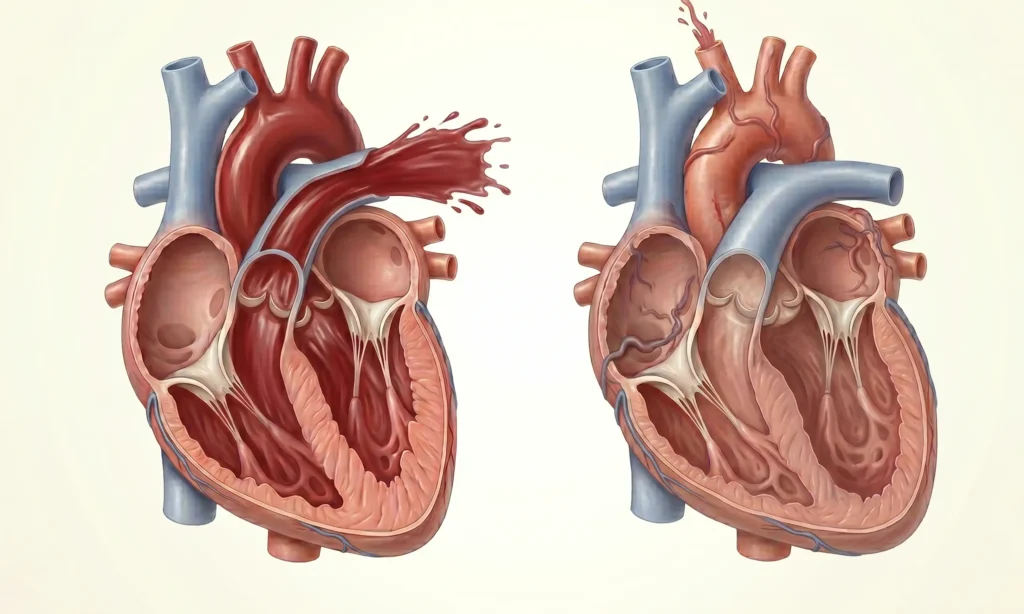
Think of your heart as a water pump. With each pump cycle, water fills the chamber — and then gets pushed out through the outlet. The pump does not push out every single drop of water in the chamber. It pushes out a portion, and the rest stays behind until the next cycle.
Ejection Fraction measures that portion — specifically, what percentage of the blood inside the heart’s main pumping chamber gets pushed out with each heartbeat.
The main pumping chamber of the heart is called the left ventricle. It is the hardest-working chamber — the one responsible for pushing blood out to the entire body through the aorta. When doctors talk about Ejection Fraction, they are almost always referring to the left ventricle’s EF.
Simple example: If the left ventricle fills with 100 ml of blood before a heartbeat, and pushes out 60 ml during that beat — the Ejection Fraction is 60%. The remaining 40 ml stays in the chamber. This is completely normal. The heart is not designed to empty completely with every beat.
The Ejection Fraction normal range is usually between 55% and 70% in healthy adults. This means the heart is pushing out more than half of what it fills with—which is exactly what it should be doing to keep the body adequately supplied with oxygenated blood.
When EF drops below this range, it means the heart is not pushing out enough blood per beat. The body starts receiving less oxygen than it needs — and that is when symptoms begin to appear.
Understanding the Ejection Fraction normal range helps you interpret your heart report more clearly and take timely action if needed.
What Is a Normal EF?
Understanding what different EF numbers mean helps put a report into perspective. Here is how cardiologists and heart failure specialists interpret EF ranges, based on guidelines from the American Heart Association and the European Society of Cardiology:
EF Range | What It Means |
|---|---|
55% – 70% | Normal—heart is pumping well |
50% – 54% | Slightly below normal—borderline monitor closely |
40% – 49% | Mildly reduced—heart pumping is weaker than normal |
Below 40% | Reduced EF—significant weakness, needs treatment |
Below 35% | Severely reduced—high risk, close monitoring essential |
An EF of 55 to 70 percent means the heart is pumping properly and efficiently. This is what we want to see on an echo report.
An EF between 50 and 54 is technically within or just at the lower border of normal. In isolation, it may not require treatment — but it warrants monitoring to ensure it does not decline further.
When EF falls to 40 to 49 percent, the pumping function is noticeably reduced. This range is sometimes called “mildly reduced ejection fraction” and typically signals that the heart has been under some strain—from high blood pressure, a previous heart event, or another underlying cause.
Below 40 percent, the heart is considered to have significantly reduced pumping function. This is the range associated with heart failure with reduced ejection fraction—a condition that requires active medical management.
Important: One EF number alone does not define your entire heart health. Doctors always interpret EF alongside your symptoms, your history, and other test results. A person with an EF of 45% who feels well and is being treated may be in a far better situation than the number alone suggests.
What Does Low EF Mean?
A low EF means the heart’s pumping strength has been reduced — it is pushing out less blood per beat than it should. The body, as a result, receives less oxygenated blood than it needs to function properly. Over time, this leads to the symptoms that people with heart failure experience.
Cardiologists classify this as Heart Failure with Reduced Ejection Fraction — abbreviated HFrEF. It is one of the two main categories of heart failure, and it is the one where EF measurement is most directly useful.
Common reasons for a reduced EF include:
Low Ejection Fraction (EF): What It Means
- A low EF means the heart’s pumping strength is reduced
- The heart pushes out less blood per beat than normal
- As a result, the body receives less oxygen-rich blood
- This can lead to symptoms like fatigue, breathlessness, and weakness
- Over time, it contributes to heart failure symptoms
Medical Classification
- This condition is called Heart Failure with Reduced Ejection Fraction (HFrEF)
- HFrEF is one of the two main types of heart failure
- EF measurement is most useful and directly relevant in this type
Understanding low values within the Ejection Fraction normal range helps in early detection of heart problems.
For example: A patient who had a heart attack two years ago and now has an EF of 35% — this tells us that the damaged area of the heart from the attack is contributing to reduced overall pumping function. The rest of the heart is compensating, but not fully.
What About High EF?
Many people assume that a higher EF is always better. This is a reasonable assumption — but it is not always accurate.
In some conditions, EF can appear higher than the normal range — above 75 percent. This can sometimes be seen in severe anemia, where the heart is working harder to compensate for low oxygen-carrying capacity in the blood, or in hyperthyroidism, where elevated thyroid hormone accelerates cardiac activity.
More importantly, there is a category of heart failure where EF is actually normal or even preserved—but the patient still has significant symptoms of heart failure. This is called Heart Failure with preserved ejection fraction, or HFpEF.
In HFpEF, the heart muscle becomes stiff rather than weak. It fills poorly—the ventricle does not relax and expand properly to accept blood between beats. So even though the pumping fraction looks normal or even high, the heart is not functioning well because it is not filling adequately in the first place.
This is why doctors never rely on EF alone. A normal EF does not automatically mean a healthy, well-functioning heart. The full clinical picture—symptoms, other echo measurements, patient history—always needs to be considered together.
Symptoms of Reduced EF
When EF is significantly reduced, the body begins to show the effects of inadequate blood supply. The symptoms are those of heart failure — and they appear because organs and muscles are not receiving the oxygen-rich blood they need to function properly.
Common symptoms of a reduced ejection fraction (EF) include the following:

- Shortness of breath — especially during physical activity, climbing stairs, or even simple tasks like getting dressed
- Persistent fatigue — a deep, ongoing tiredness that does not improve with rest
- Swelling (edema) in the feet, ankles, or legs — due to fluid buildup when the heart cannot pump effectively
- Fast or irregular heartbeat (palpitations) — the heart tries to compensate by beating faster
- Difficulty lying flat (orthopnea) — breathlessness worsens when lying down due to fluid shifting to the lungs
- Reduced ability to exercise or perform daily activities that were previously easy
These symptoms commonly appear when the value falls below the Ejection Fraction normal range.
For example : a patient with an EF of 38% may find themselves breathless after walking to the kitchen, swollen in the legs by evening, and unable to sleep lying flat. These are classic symptoms of reduced EF causing heart failure symptoms.
These symptoms occur because less blood is reaching the body with each heartbeat. The brain, muscles, kidneys, and other organs are working with a reduced supply and they communicate that deficit through these recognizable symptoms.
How Do Doctors Measure EF?
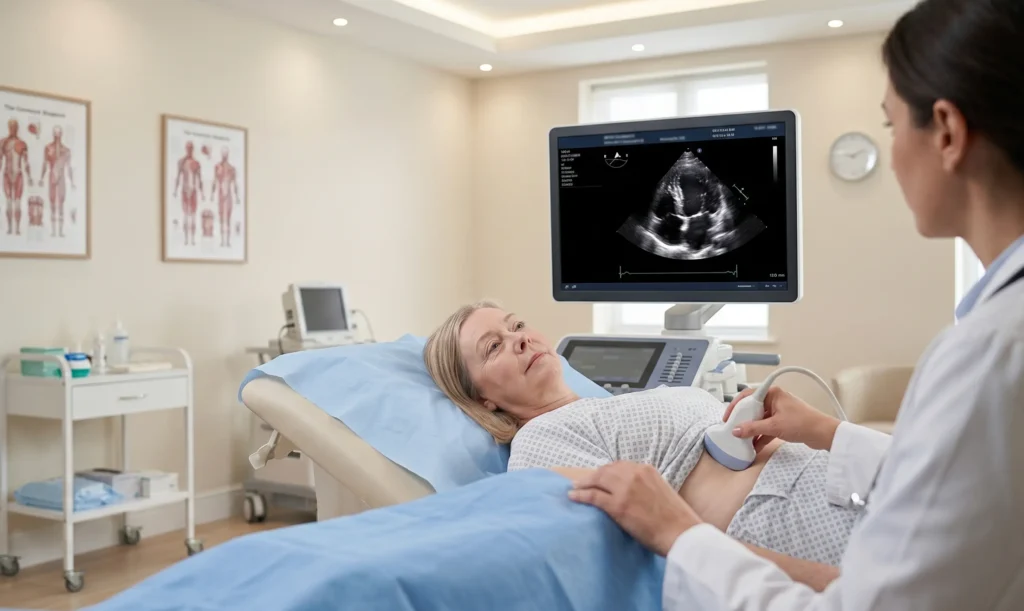
The most common and widely used test for measuring EF is the echocardiogram—simply called an Echo. It is a heart ultrasound that uses sound waves to create real-time moving images of the heart in action. A small handheld probe is placed on the chest wall, and from the images it produces, cardiologists can directly visualize and calculate how much the left ventricle contracts with each beat.
The echocardiogram is completely painless, involves no radiation, takes about 30 to 45 minutes, and provides an enormous amount of information about heart structure and function — not just EF. It is the single most useful non-invasive test in cardiology.
Other methods used to measure EF when more detail is needed include:
- Cardiac MRI — the most accurate method, providing highly detailed images of heart muscle structure and function
- Nuclear scan (MUGA scan) — uses a small amount of radioactive tracer to track how blood moves through the heart
- CT scan — can estimate EF as part of a broader cardiac assessment
- Cardiac catheterization — an invasive test, used when other methods are not sufficient or when treatment planning is needed
For the majority of patients, the echocardiogram provides everything the cardiologist needs. The other methods are typically used in specific clinical situations requiring more detailed assessment.
These tests help determine whether your heart is within the Ejection Fraction normal range.
Can EF Improve?
Yes—and this is one of the most important and encouraging messages in modern heart failure medicine. EF is not a fixed number. In many patients, with the right treatment and lifestyle changes, EF improves significantly over time.
The extent of improvement depends on the underlying cause, how early treatment is started, and how consistently the patient follows their treatment plan. But meaningful improvement — sometimes from 30 percent up to 50 percent or more — is genuinely achievable in many cases.
Medications Used to Improve Ejection Fraction (EF)
- ACE inhibitors or ARBs — reduce the pressure the heart pumps against, helping decrease workload and improve efficiency
- Beta blockers — slow the heart rate and allow better filling, reducing strain on each heartbeat
- SGLT2 inhibitors — a newer class of medicines (originally for diabetes) that have been shown in large studies to improve outcomes in heart failure with reduced EF
- Diuretics — help remove excess fluid from the body, reducing swelling and relieving breathlessness
The goal of treatment is to improve heart function, relieve symptoms, and bring it closer to the Ejection Fraction normal range.
When medicines alone are not sufficient, device therapy may be considered. An ICD—Implantable Cardioverter Defibrillator—protects against dangerous heart rhythm disturbances that are more common when EF is very low. A CRT device — Cardiac Resynchronization Therapy — helps the two sides of the heart beat in a coordinated way, improving overall pumping efficiency.
Lifestyle changes are not optional extras in this process—they are essential. Patients who combine their medicines with a heart-healthy diet, appropriate exercise, salt restriction, and complete abstinence from alcohol and smoking consistently achieve better outcomes than those who rely on medicines alone.
How to Protect Your Heart and Ejection Fraction (EF)
Whether your EF is currently normal and you want to keep it that way, or whether you are working to improve a reduced EF—the following steps are supported by strong evidence and recommended by international cardiac guidelines.
Following these steps consistently helps maintain the Ejection Fraction normal range over time.
- Control blood pressure: Long-term high BP weakens the heart. Keep it in the target range with medicines and lifestyle
- Manage diabetes carefully: High blood sugar damages blood vessels and heart muscle over time
- Stop smoking completely: There is no safe level of tobacco use for the heart
- Reduce salt intake: Too much sodium causes fluid buildup and increases strain on the heart
- Exercise regularly: At least 30 minutes of brisk walking most days helps strengthen the heart
- Maintain a healthy weight: Obesity increases the risk of hypertension, diabetes, and cardiomyopathy
- Limit or avoid alcohol: Early stopping can reverse alcohol-related heart muscle damage
- Take medicines as prescribed: Regular use improves outcomes and prevents worsening of heart function
When Should You Get EF Checked?
Not everyone needs an echocardiogram routinely. But there are specific situations where checking EF is important and medically recommended:
- After a heart attack: EF helps guide treatment decisions and assess risk
- If you have symptoms of heart failure: breathlessness, leg swelling, fatigue, or difficulty lying flat
- If you have long-standing uncontrolled high blood pressure
- If you are on treatment for heart failure: EF monitoring shows whether treatment is working
- If your doctor finds abnormal heart sounds or rhythm changes during examination
- Before and during chemotherapy: some cancer medicines can affect heart function, so EF monitoring is important
In patients already diagnosed with reduced EF, cardiologists typically repeat the echocardiogram every 6 to 12 months — or sooner if symptoms change — to track response to treatment and adjust the management plan accordingly.
Frequently Asked Questions (FAQ)
Q1. Is low EF dangerous?
Low EF can be serious, but it depends on how low the value is and whether symptoms are present. Many people live stable, active lives with reduced EF when it is properly diagnosed and treated. It should be taken seriously, but it is not a life sentence.
Q2. Can EF improve?
Yes, in many cases EF can improve significantly. With the right medicines and lifestyle changes, improvement can occur over months to years. Early treatment makes the biggest difference.
Q3. Is a normal EF equal to a healthy heart?
Not always. Conditions like HFpEF, valve disease, and coronary artery disease can still be present even with a normal EF. That is why an echocardiogram report should always be interpreted along with symptoms and full medical history.
Conclusion
Ejection Fraction is a simple number, but it reflects how well your heart is pumping. A normal EF is a good sign, while a low EF means your heart may need attention.
The good news is that with proper treatment and lifestyle changes, EF can often be improved or managed. If your report shows a low EF or you have symptoms, do not ignore it — early action makes a real difference.
Medical Disclaimer
This article is written for general educational awareness only. It does not constitute medical advice, diagnosis, or treatment recommendation.
If you have received an echocardiogram report showing reduced EF, or if you have symptoms of heart failure, please consult a qualified cardiologist for proper evaluation and personalized care.
About the Author
Iraphan Khan, BSN, NP, is a Public Health Researcher and Healthcare SEO Strategist at RealMedVision. He creates medically accurate, evidence-based content for clinics and health brands.
Medically Reviewed By
Dr Praveen Verma MBBS MD — Diagnostic & Pathology
Dr Himanshu Morya MBBS — Clinical Accuracy & Patient Safety
Kalpna Singh Shekhawat BSN NP — Patient Care & Practical Accuracy
References:
American Heart Association (AHA) ECG Guidelines | World Health Organization (WHO) | National Institutes of Health (NIH) | Mayo Clinic | American College of Cardiology (ACC) | Rapid Interpretation of EKGs — Dale Dubin
